 Multiple lights or devices can be used to manage high SBR levels. 
The type of light used is determined by the type and levels of jaundice. Two types of phototherapy devices are available. The effects of phototherapy are reversible, so when the light is turned off, the bilirubin transforms back to a fat-soluble molecule. Phototherapy simply converts unconjugated bilirubin into photoisomers of bilirubin, which are water soluble and excretable via the liver into the small bowel. Phototherapy is the usual treatment for neonatal jaundice and it is used to curtail the rise of unconjugated bilirubin therefore preventing kernicterus. Babies with rapidly increasing SBRs or potentially in need of an exchange transfusion should be cared for on the neonatal unit. Careful plotting of SBR levels on treatment threshold graphs for the infant’s gestation will indicate the when the baby requires phototherapy or an exchange transfusion. It is also important to ensure that the infant’s stages of metabolism are supported by ensuring the baby is given adequate food (glucose is needed for conjugation) and drink (to ensure excretion and minimise enterohepatic shunting). If the underlying cause of jaundice is treatable then this should be treated. Jaundice should be quantified and this can be done by transcutaneous devices and blood sampling. Jaundice develops in a ‘head to tail’ direction – first the head, then body and finally the limbs. 
The sclera or ‘white’ of the eye and skin when pressed will be yellow. Jaundice can be assessed by examining the skin and eyes. National guidelines are available and include treatment thresholds/graphs and algorithms on investigations, management of jaundice, including phototherapy and exchange transfusions. Assessment and management is essential to prevent these complications. High levels of unconjugated bilirubin can result in damage to the basal ganglia in the brain causing kernicterus and damage to the 8th cranial nerve, resulting in sensorineural hearing loss. As the breast-fed baby is more efficient at absorption, the overall result is an increase in enterohepatic shunting. Breast milk contains high levels of β-glucuronidase, increasing the cleaving of conjugated bilirubin/urobilinogen back to unconjugated bilirubin. Small-volume feeds result in less frequent and smaller stools, increasing enterohepatic shunting, and a caloric deficiency, increasing circulating free fatty acids which can displace unconjugated bilirubin from albumin.īreast milk inhibits the development of bacterial gut flora and the making of urobilinogen. Mothers do not initially produce sufficient quantities of milk for the demand-fed infant unlike bottle-fed infants who are given calculated amounts at regular intervals. Feeding stimulates the gastrocolonic reflex and increases intestinal motility, clearance of meconium and conjugated bilirubin from the gut. The impact of feeding frequency can be a contributing cause of jaundice in the breastfed baby. The use of early versus late onset is preferred by many over using the terms physiological or pathological jaundice. It is important not to imply that breast milk jaundice is harmful, thereby influencing a mother’s choice not to breastfeed. There is controversy in the literature as to how to classify breast milk jaundice. Causes of physiological and pathological jaundice can be linked to each stages of metabolism ( Table 64.2). Pathological jaundice can present on day 1 or it can be prolonged, persistent after day 14 in the term infant or day 21 in the preterm infant. Pathological jaundice, on the other hand, should raise concern and always requires further investigation. Serum bilirubin (SBR) levels will peak by day 4 and reduces by day 14. Jaundice is classified as physiological or pathological. Physiological versus pathological jaundice 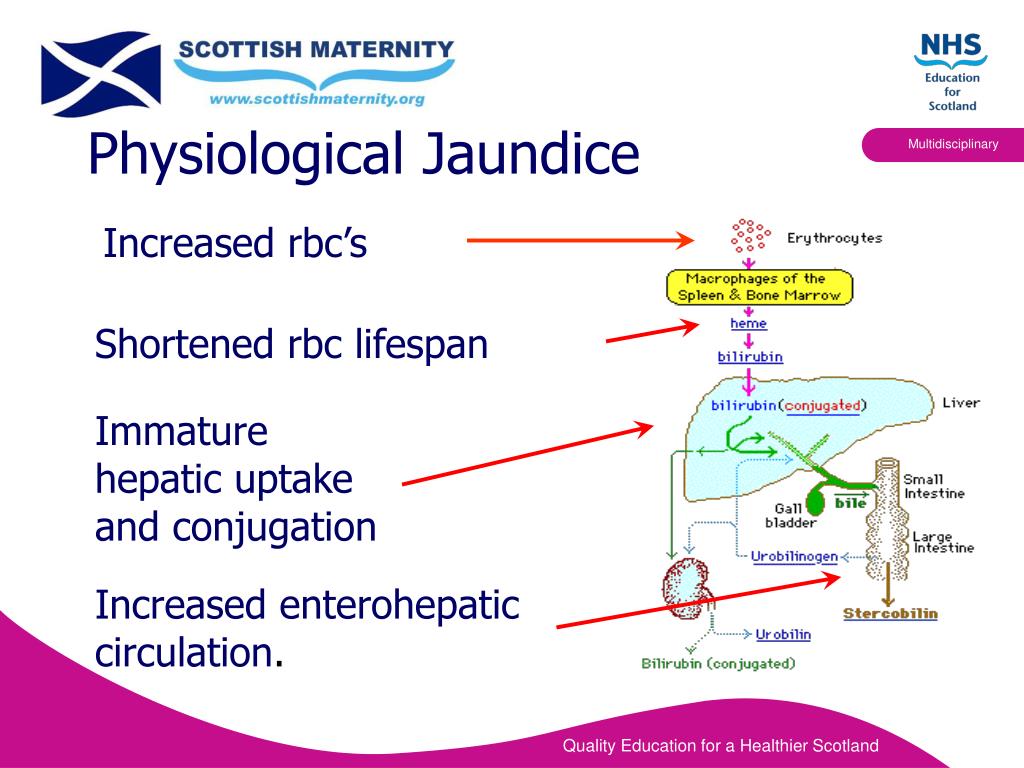
Alterations at any of these stages can result in jaundice ( Table 64.1). There are four stages involved in bilirubin metabolism. In order to provide informed care for a jaundiced baby and parents it is important to have an understanding of bilirubin metabolism. 
Jaundice in the newborn is common, occurring in over two-thirds of term infants and even more frequently in the preterm infant. Jaundice occurs when bilirubin accumulates in the extravascular fatty tissues (skin and brain). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
